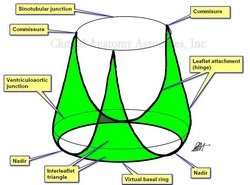
Interleaflet triangles of the aortic valve by MTD.
Click for a larger image.
The interleaflet triangles (ILTs) are three triangular regions found in the ventricular aspect of the aortic root. They are bound inferiorly by the virtual basal ring (VBR), laterally by the attachment of the leaflets (the hinge) to the aorta and left ventricular wall (muscular and fibrous), and superiorly by the commissures (site of attachment and meeting of adjacent leaflets) which are usually located at the sinotubular junction, also known as the sinotubular ridge.
A review of the literature on the topic shows that although many speak of these ILTs, not many authors have clearly defined their boundaries. In fact, some only reserve the term ILT to the triangular region distal to the ventriculoaortic boundary. The description used in this article includes the ventricular wall found between the VBR and the ventriculoaortic junction as well as fibrous components found between these two boundaries. Based on this description, we have developed an image of the ILTs that, to our knowledge is not found in literature. (see accompanying images).
The virtual basal ring is a circular virtual line formed by the nadirs of the three aortic leaflets (cusps). The attachment of the three leaflets create a three-pronged coronet that is useful in defining the interleaflet triangles (see image)
The superior boundary of the ILTs is formed by three commissures, the points where the leaflets meet each other at the sinotubular junction. There are two posterior commissures, right and left. The right-posterior commissure is found between the noncoronary and the left coronary sinuses (of Valsalva). An important point about this commissure is that it is situated above the midpoint of the septal (anterior) leaflet of the mitral valve. The left-posterior commissure is found between the left and the right coronary sinuses. The anterior commissure is located between the right and the noncoronary sinus close to the membranous interventricular septum.
Based on the above description, there are three interleaflet triangles:
a. Right (posterior), left (posterior), and anterior. The right posterior ILT is located between the noncoronary and the left coronary sinuses, and just as the commissure at its apex, is located at the midpoint of the septal (anterior) leaflet of the mitral valve. Also, the superior aspect of this ILT is related to the transverse pericardial sinus.
b. The left posterior ILT is located between the right and the left coronary sinuses, and is lies immediately behind the right ventricular outlet.
c. The anterior ILT is found between the right and the noncoronary sinuses. It is related to the membranous septum and the right fibrous trigone, forming part of the central fibrous body (skeleton) of the heart. This ILT is a good anatomical landmark to the location of the bundle of His and the left bundle branch, both components of the conduction system of the heart. These structures can be compressed during the implantation of an aortic or mitral valve, causing transitory or permanent cardiac conduction problems.
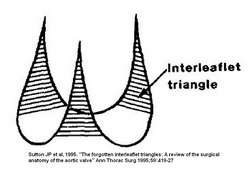
Interleaflet triangles of the aortic valve by Sutton.
Click for a larger image.
The ILTs are important in the normal physiology and hemodynamics of the aortic valve. A small ILT will affect the diameter of the valve and the movement of the leaflets, causing stenosis. This is the case in bicuspid aortic valves where the fusion of two of the leaflets leads to the reduction in size of the ILT normally found between these two fused leaflets.
Since they are located within the functional portion of the left ventricle, the ILTs are subject to the pressures of the ventricle and can be areas that develop aneurysms.
Because of their importance in the hemodynamics of the aortic valve, new procedures and medical devices that reshape the ILTs are being developed. This is specially important in the case of a bicuspid aortic valve, where the interleaflet triangles may be abnormal.
Further to the images that are depicted in this article, the lower image is the classic image of the interleaflet triangles by Sutton (1995). As you can see, the base of the triangles is shown straight with no clear boundary, and it seems as though they are related to the ventriculoaortic junction. The nadirs are not used as a point of reference. The upper image (developed by us and based on Sutton's original sketch) clearly shows the extent of the ILTs as well as their relation to the three landmarks that define the aortic root: The virtual basal ring, the ventriculoaortic junction, and the sinotubular junction.
NOTE: The pulmonary valve also has interleaflet triangles, with a somewhat similar description, but since they are under low pressure they do not develop or are cause of pathology as the ILTs of the aortic valve.
Sources:
1. The Anatomy of the Aortic Root: Loukas, M et al. Clinical Anatomy 27:748–756 (2014)
2. “Extracardiac aneurysm of the interleaflet triangle above the aortic-mitral curtain due to infective endocarditis of the bicuspid aortic valve.” Hori D, et al. Gen Thorac Cardiovasc Surg. 2008 Aug;56(8):424-6
3. “Anatomy of the aortic root: implications for valve-sparing surgery” Efstratios I. Charitos, HS. Ann Cardiothorac Surg 2013;2(1):53-56
4. “The Forgotten Interleaflet Triangles: A Review of the Surgical Anatomy of the Aortic Valve” Sutton JP, et al Ann Thorac Surg 1995;59:419-27
5.” The aortic interleaflet triangles annuloplasty: a multidisciplinary appraisal” Mangini, A., et al. European Journal of Cardio-Thoracic Surgery, Vol. 40:4, 2011, 851-857
6. “Structure and Anatomy of the Aortic Root” Ho, SH., Eur J Electrocar 2009 10; i3-i10
7. “In vitro study of the aortic interleaflet triangle reshaping” Vismara, R Journal of Biomechanics; 47:2; 2014. 329-33




